Hello, pump: Returning to work while breastfeeding
You are a breastfeeding mom. And you’re also an employee or a student, heading back to work or school. You’re thinking, wondering, worrying: “um, how is this going to happen, exactly?!” Combining nursing with returning to work after maternity leave is definitely a challenge, but for many moms, it’s absolutely doable with some organization and persistence. Perhaps the most important thing is to remember to figure out what is going to work for you and your family, not some hazy ideal. “Your worth as a mother is not measured in ounces,” says Jessica Shortall, author of Work. Pump. Repeat: The New Mom’s Survival Guide to Breastfeeding and Going Back to Work (Abrams Books) and mom of two. “You’re doing a really hard job. Be kind to yourself.”
Here’s what you need to know about breastfeeding, pumping and going back to work.
Have the boob talk with your boss
Before or during your mat leave, talk to your supervisor or your Human Resources department about pumping and storing breast milk while at work. In the United States, if you are an employee covered under the federal Patient Protection and Affordable Care Act (ie if you are eligible for overtime and your company has over 50 employees), your workplace is required to give you reasonable breaks to express breast milk, in a private area that is not a bathroom. Workplaces with fewer than 50 employees must prove that giving employees breaks for pumping breast milk causes “undue hardship.” Check this Department of Labor link for more information.
If you are not covered under the PPACA, the laws in your state may still protect your access to time to pump without penalty, so it’s best to check with state legislation. “I find that most employers are not trying to give employees a hard time about pumping breaks,” says Wendy Wright, an International Board Certified Lactation Consultant (IBCLC) and co-founder of Lactation Navigation in Palo Alto, California, which specializes in nursing working moms. “Once they understand that you need to pump every three hours to keep your milk supply up, rather than just pumping at home, they get on board and are supportive.”
In Canada, most women take up to a year of maternity leave before returning to work. If they return to work or school earlier, there isn’t specific provincial legislation in place regarding time to pump, but the Canadian Human Rights Act protects all federally regulated employees from pregnancy-related discrimination, including breaks for pumping.
Getting ready: Pumping and storing
Many working moms prefer the efficiency of a double electric pump that pumps both breasts at once in about 10-20 minutes—check with your insurance company to see if a pump purchase or rental is covered.
Mat leave lengths vary, but many IBCLC recommend giving yourself at least four weeks to adjust to breastfeeding and getting to know your baby before you start thinking about pumping and storing milk. “Starting to pump 10 to 15 days before you go back to work is generally enough time to build up a small supply of stored breast milk,” says Wright. “We say pump once a day for 15 minutes at first—no pressure, no expectation—to set up a positive relationship with the pump. We tell moms to aim initially for one ounce a day, which most can achieve no problem. It’s nice to go back with 20-25 oz in the freezer.” Label the packaged milk with the date, and use the older milk first.
According to lactation consultants, a good guideline is to leave 1 oz of milk per hour for the time you will be away from your baby. So if your workday and commute is 9 hours, you give your child care provider 9-10 oz of expressed breast milk for your baby to drink over several feedings throughout the workday.
A pattern that works for many moms with a Monday to Friday workweek is to take frozen milk and put it in the fridge to thaw on Sunday night. This milk goes to the caregiver on Monday. You pump at work on Monday and give that milk to the caregiver at pickup on Monday night for use on Tuesday, and so on. On Friday night, package milk into 1-2 oz containers, date it and freeze it. Breastfeed every morning and evening, and overnight if your baby is waking to nurse, as well as on demand on your days off.
Preparing to go back
Once breastfeeding has been established, around four to six weeks, it’s fine for your partner or another caregiver to give the baby a bottle of expressed breast milk. “Choose a nipple labelled ‘very slow flow,’ ” advises Sarah Tyack, a registered nurse and IBCLC in Seattle, Washington, who works with nursing moms through her company Babe N’ You. This helps you mimic the breast as much as you can, she says, so your baby doesn’t get used to chugging an easy-flow bottle and then not want to work a bit more when it’s time for breastfeeding.
Day care providers may not be used to babies who drink breast milk. “Feeding too much at day care is the biggest ‘booby trap,’” says Tyack. “Then the baby isn’t that hungry at the end of the day and doesn’t nurse much, so mom’s milk supply goes down and it gets into a cycle. Also, a baby may want to suck but there are other ways to soothe a baby other than a bottle—using a pacifier, for example.” She recommends that the caregiver provide the last bottle two hours or more before pickup, and then you can nurse when you arrive at the day care or in your own home. When choosing a caregiver, Wright suggests asking questions like, “Will you refrigerate and reuse any leftover breast milk?” and “Do you require all parents to clearly label milk containers to avoid mix-ups?”
Create a breastfeeding calendar
Wright is a big fan of a calendar because it helps to give parents and caregivers some sense of what to expect. “The 12-week mark is a very common growth spurt and baby is hungry. If you know it’s coming, you can tentatively book a half-day off, or plan to come to the day care at lunch to nurse, or have your mother-in-law bring the baby to you at lunch,” she says. “Taking time off at strategic times gives you a little more power.” Similarly, if your baby is five months old and you’re wondering if you can continue pumping enough breast milk, knowing that the six-month mark for introducing some solids (in consultation with your health care provider) is on its way can be inspiring.
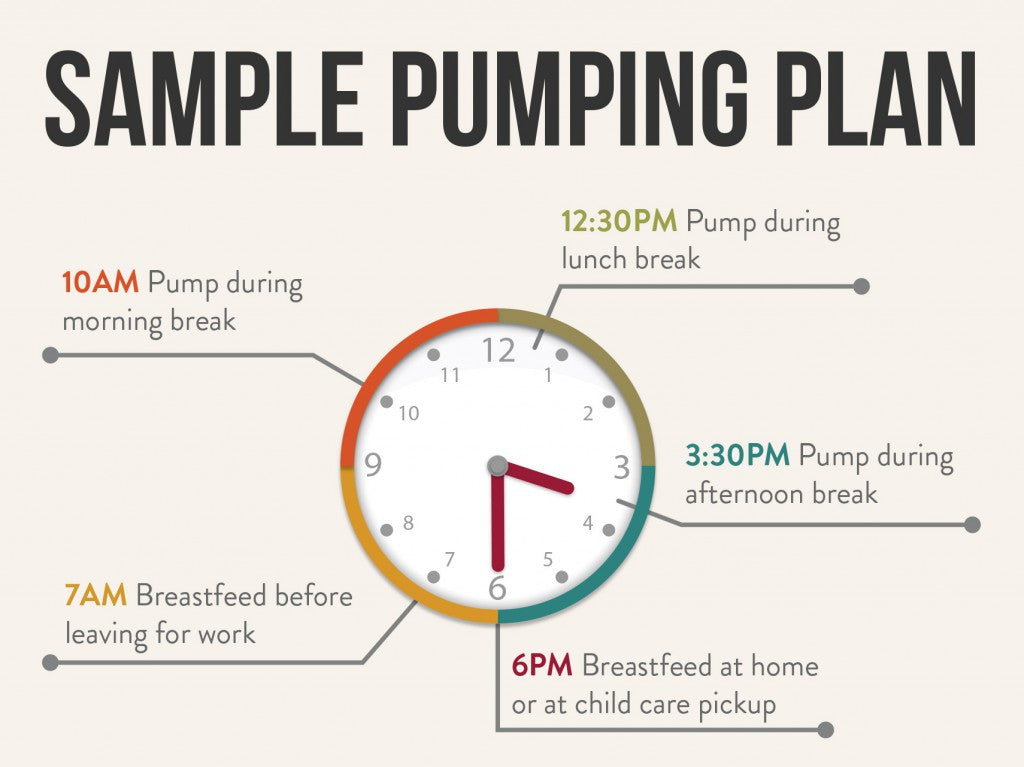
Sample Pumping Plan
Pumping at work
So you’re back at work, you’re wearing your breastfeeding top and it’s time to pump: is your body going to cooperate? “It’s common for your milk supply to decrease when you’re away from your baby, so it’s important to pump every three hours,” says Tyack. She suggests looking at your baby’s picture, bringing a blanket or onesie that has that baby smell and even listening to a recording of your baby’s burbles and coos to help with milk flow. Wright suggests massaging and compressing your breasts while the pump is working. “You get more milk, and you empty your breasts more completely which is definitely more comfortable,” she says. “Clients tell me that when they compress the breast and see more milk flow into the pump, they feel more powerful and more trusting of their body.”
Ok, you’ve got the expressed milk—now what? The milk goes in the fridge or a cooler with ice packs until you head home. Some women like to use specially formulated wipes to clean their pump before storing it. You can also just put the whole pump into a self-sealing plastic bag (if it’s a shared fridge you can use an opaque self-sealing bag, available online) and stash it in the fridge until you’re ready to take it home in a cooler. “Breast milk keeps for six days in the fridge, so as far as I’m concerned you can wash your pump once or twice a week and be totally fine,” says Tyack.
Shortall, who returned to work as a charitable director for a shoe company when her kids were 12 and 16 weeks old respectively, has lots of real-life ideas for making pumping work at work. Some she uncovered on her own while pumping and travelling internationally for work (sometimes to rural Nepal!), and others she learned by talking to moms who pumped during their jobs as police officers, doctors, teachers or executives. Some examples: “If you are traveling for work and have to pump sitting on a public toilet—which will happen—put a post-it note over the auto flush sensor to stop it from flushing on your butt,” she says. She discovered that the pump flange is a great funnel for pouring milk from bottles to bags for freezer storage. If a hotel won’t give you a room with a fridge on a business trip, tell them you need it to keep “medicine” cold.
And while combining pumping with working is sometimes tough and stressful, it’s rewarding—and it brings the unexpected too. “I was pleasantly surprised to find so many helpers along the way,” notes Shortall. “From young, male employees who didn’t bat an eye or ask why (after the first time) when I abruptly left meetings, to co-workers who brought me nutritious snacks because they knew that pumping was cutting into my ability to sit and eat lunch…there are a lot of great people out there.”